Introduction
Fibroids are an enormous healthcare problem because they are the primary reason given for surgery in 199,000 hysterectomies and 30,000 myomectomies performed yearly in the US. The cost of inpatient surgery for fibroids is about $2 billion a year. Time taken away from work or family make this condition very costly for women and their families. And, presently there are many options other than hysterectomy available for women with bothersome fibroid symptoms.
Women and their gynecologists need better information on which to base decisions regarding possible treatments. Hopefully, this website will provide you with that information. Much of the information on this website is adapted from two articles I recently published in the prestigious international journal Fertility and Sterility: Etiology, symptomatology, and diagnosis of uterine myomas and Uterine myomas: management. These two articles are the result of reading more than 300 research papers about fibroids. This is information you will want to know before choosing the path to take for any fibroid-associated problems.
What Are Fibroids?
Fibroids are non-cancerous (benign) growths of the muscle wall of the uterus. They are probably responsible for more unnecessary gynecologic surgery than any other condition. Every year a staggering 600,000 American women have a hysterectomy. And about 30 percent of those hysterectomies, 199,000 in all, are performed because of fibroids. Many of these surgeries are not necessary.
Fibroids are extremely common. More than 75 percent of women can be found to have small fibroids using MRI, a very sensitive imaging technique. However, only about 30 percent of all women will have fibroids large enough to be noted during a pelvic exam, and the vast majority of even these women, more than 80 percent, will never have symptoms and will never require treatment. And for the rare woman who does have problems, there are a number of sound and effective options available. Hysterectomy should be the solution of last resort.
What Causes Fibroids?
While there is much we don’t know about fibroids, we do know that each individual fibroid starts from a single cell growing abnormally (mutation). These cells overproduce large amounts of collagen and other proteins. Recently, other gene mutations have been discovered in fibroid cells that alter the cell’s growth. There may also be environmental causes, as yet undetermined, that stimulate fibroid growth. It is important to realize that there is no evidence that fibroids turn into cancer. Fibroids are benign from the beginning and remain benign.
We do know that the female hormones estrogen and progesterone are necessary for fibroids to grow, but growth of a fibroid requires a complex interaction of estrogen, progesterone, and cell growth factors. Fibroids do not occur before puberty when estrogen and progesterone production begins, and fibroids shrink after menopause when hormone production drastically decreases. Studies are now under way to try to determine how fibroids start and what influences their growth.
Fibroids usually do not develop until between ages twenty-five and thirty-five. You might expect that women with fibroids are making too much estrogen or progesterone, however the levels of these hormones in the blood are absolutely normal. But, fibroids have enzymes that convert androgens (male hormones made by the ovary and the adrenal gland) into estrogens within the fibroid cells, so the fibroid cells actually contain higher levels of estrogen than the the rest of the body. Fibroids are also very sensitive to progesterone and appear to thrive during the time of the menstrual cycle when progesterone levels are highest.
Special proteins found in the bloodstream, called growth factors, are produced by cells in the body and stimulate fibroid growth. Some of the identified fibroid-related growth factors (which sound like a virtual alphabet soup) are transforming growth factor-B (TGF-B), basic fibroblast growth factor (bFGF), epidermal growth factor (EGF), platelet derived growth factor (PDGF), vascular endothelial growth factor (VEGF), insulin-like growth factor (IGF) and prolactin (PRL). Some of these growth factors encourage cell growth and others encourage blood vessel growth to feed the fibroids. Unfortunately, we still do not understand which of these proteins are important.
Importantly, women with fibroids are not more prone to fibrocystic changes in the breast, a totally unrelated condition and they are not more prone to develop any other benign or cancerous conditions.
How Common are Fibroids?
Fibroids are extremely common. One study found fibroids, some as small as ¼ inch, in 77% of women. Because ultrasound cannot see these small fibroids we often underestimate how common this condition is. Small fibroids, however, are almost never bothersome. By age 35 fibroids can be found using ultrasound in 60% of African-American women and 40% of Caucasian women. By age 50, fibroids can be found in 80% of African-American women and 70% of Caucasian women.
What Increases Your Risk for Developing Fibroids?
Studies that evaluate “risk factors” are very hard to do, so we don’t really know how important these factors are.
- If you have a mother or sister with fibroids, you have an increased risk.
- African-American women have a higher risk than Caucasian women.
- Using birth control pills does not appear to increase risk, except very rarely.
- Pregnancy and childbirth decrease the risk.
- Smoking decreases the risk (but, not a reason to smoke!)
- Hormone therapy after menopause usually does not make fibroids grow.
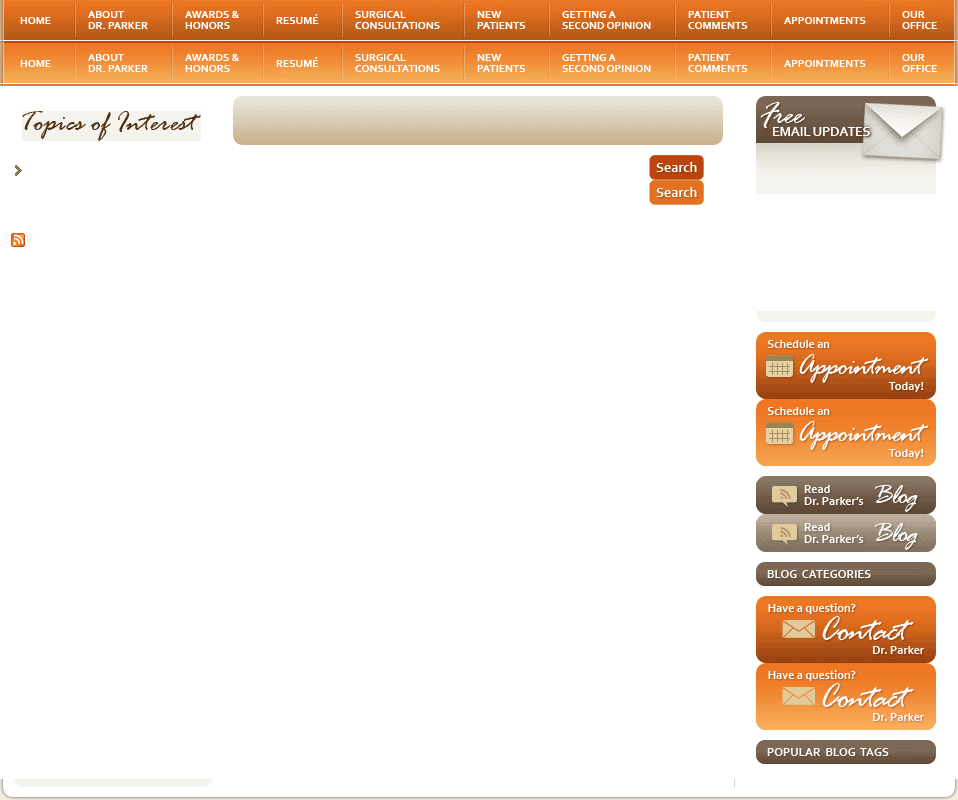
What Are the Different Types of Fibroids?
All fibroids begin as a growth somewhere within the uterine muscular wall. The symptoms caused by fibroids depend on where they grow in the wall and how big they are. Fibroids that grow and bulge toward the outside of the uterus, called subserosal fibroids, can press on (but not injure) the organs surrounding the uterus such as the bladder or rectum. Sometimes, they may grow large enough to push outward and cause a noticeable swelling in the abdomen.
Fibroids that grow and bulge toward the inside of the uterus are called submucosal fibroids. These grow directly below the lining cells of the uterus and may lead to heavy or irregular bleeding. Fibroids that stay mostly embedded within the middle of the wall of the uterus are called intramural fibroids. Some fibroids may form on stalks that connect them to the uterus. These are called pedunculated fibroids and can be either submucosal or subserosal in location.
What is the Best Way to Make the Diagnosis of Fibroids?
Fibroids are most commonly diagnosed during a pelvic examination. Fibroids are benign tumors of the uterine muscle wall and, as such, cause the uterus to feel larger than normal and irregular. If the size of the uterus is hard to determine or the diagnosis is uncertain, a pelvic ultrasound can be helpful. An ultrasound exam is fairly accurate at determining the sizes and positions of fibroids within the uterine wall. However, sometimes the exact position of the fibroids is hard to accurately determine with ultrasound.
The best test to tell size and position of fibroids is an MRI. Fibroids contain more collagen than normal uterine muscle and, as a result, the fibroids appear distinct and darker on the MRI. Getting an MRI may be a good idea if the ultrasound is not clear or it is important to know exactly where the fibroids are. I also use this test if a laparoscopic myomectomy is being considered. MRI gives me a good idea as to whether it will be possible to get all the fibroids out with the laparoscopic instruments. If ultrasound is not clear, MRI can also be used to see if submucous fibroids are present. This can be helpful if unexplained heavy bleeding is present or fertility is a concern.
What size are my fibroids?
Gynecologists and ultrasound reports usually describe the size of fibroids using centimeters (cm), a measurement unfamiliar to most Americans. Often, a comparison to fruits or common objects can help to understand the size. We also compare the size to weeks or months of pregnancy, since many women are familiar with this measurement. The following measurements may help:

Pea = 1 cm
-

Grape = 2 cm
-

Walnut = 3.5 cm

Plum = 5 cm

Orange = 6.6 cm

Baseball = 7.5 cm

Grapefruit = 10 cm

Cantaloupe = 12 cm

Honeydew melon = 16 cm
William H. Parker, MD
Clinical Professor, Reproductive Medicine, UC San Diego School of Medicine
Page last updated: January, 2018