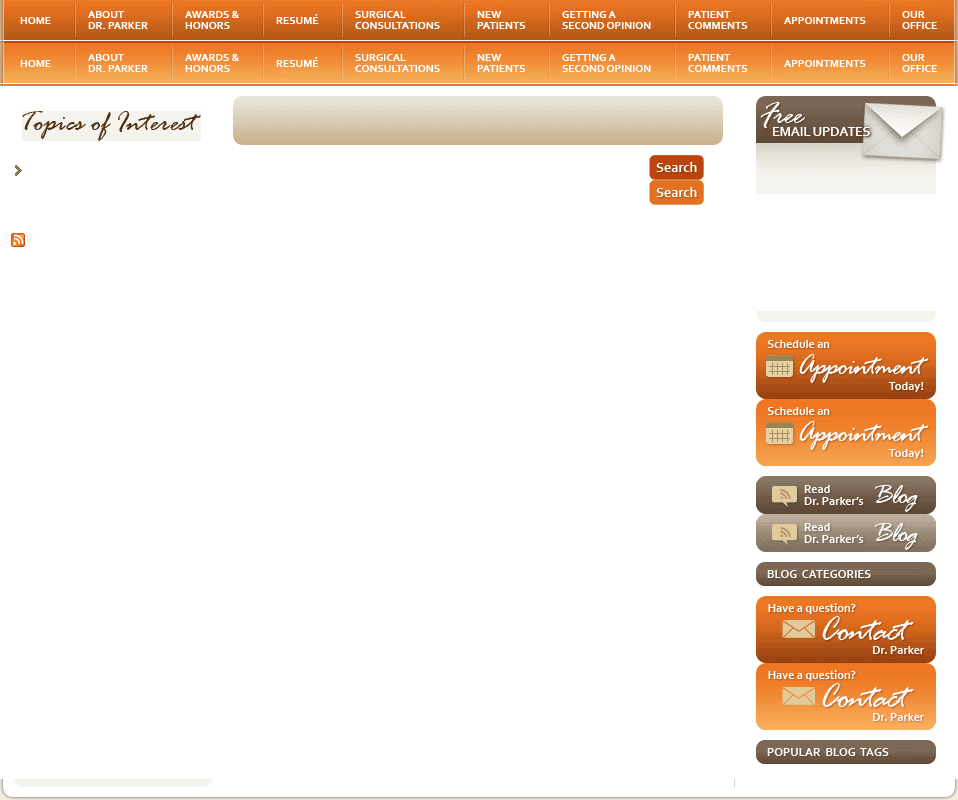
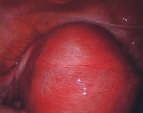
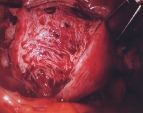
Adenomyosis is a non-cancerous condition of the uterus that can mimic many of the signs and symptoms of fibroids. This condition results from the lining cells of the uterus growing directly into the muscle wall of the uterus. When the lining cells of the uterus bleed at the time of the menstrual period, these misplaced cells in the muscle bleed as well. And bleeding directly into the muscle causes pain. As the blood accumulates, the surrounding muscle swells and forms fibrous tissue in response to the irritation. This swollen area within the uterine muscle wall, called an adenomyoma, feels very much like a fibroid on examination and is often confused with a fibroid on a sonogram. Adenomyosis may be mild and cause no symptoms at all, or, in more severe forms, it may lead to heavy bleeding and severe cramping during menstrual periods. Adenomyosis is present in about 10 percent of women and, therefore, is less common than fibroids.
How Is the Diagnosis of Adenomyosis Made?
The diagnosis of adenomyosis is suspected if the uterus feels enlarged and tender to the touch during the pelvic examination. However, the diagnosis of adenomyosis based on these findings is often inaccurate, and other causes-fibroids, endometriosis, or polyps-are often found as the cause for the bleeding or discomfort. The diagnosis may be suggested by the appearance of the uterus on a sonogram, although it is often difficult to tell the difference between adenomyosis and fibroids using sonography. MRI is better at detecting adenomyosis, but the test is very expensive and rarely used for this purpose. Unfortunately, the only way to establish the diagnosis of adenomyosis with certainty is with surgery. Once removed, the tissue can be examined under the microscope, and the uterine lining cells can be seen within the muscle wall.
Adenomyosis and Infertility
Journal: Obstetrics and Gynecology International, 2012
Authors: Campo S, Campo V, Benagiano G.
Study from: Catholic University of Sacred Heart, Roma, Italy.
Problem: Adenomyosis is a benign condition where the uterine lining cells grow deep into the uterine muscle wall. For many years, adenomyosis has been suspected of causing infertility in women. In the past, the diagnosis of adenomyosis has only been possible based on a pathologist’ examining the uterine muscle and lining cells after a hysterectomy, so fertility could never be measured. Now MRI (and probably 3-D ultrasound) allows the diagnosis of adenomyosis without hysterectomy and, therefore, scientific investigation of this condition has increased dramatically.
Study: The authors reviewed the new research and they present multiple reasons why adenomyosis might cause infertility.
Results: The evidence that adenomyosis causes infertility includes:
- In women with adenomyosis, the muscles cells in the uterine wall swell and they function differently than normal uterine muscle cells.
- In women with adenomyosis, the lining cells of the uterus do not go through normal changes during the menstrual cycle.
- In women with adenomyosis, the uterine lining cells cause inflammation in the muscle wall which interferes with the movement of the fertilized egg inside the uterus.
- In women with adenomyosis, there are changes in the uterine lining cells that interfere with implantation of the fertilized embryo.
- Surgical removal of adenomyosis or medical treatment with GnRH agonists (Lupron) increases the chance of pregnancy.
Dr. Parker’s Comments: In order to prove that adenomyosis causes infertility, a large group of women would need to have an MRI before trying to get pregnant and the percent of women who get pregnant with adenomyosis would need to be compared with the percentage of women who do not have adenomyosis. Since that type of study has never been done, it is currently impossible to prove that adenomyosis can lead to infertility. However, now that women with adenomyosis can be diagnosed by MRI, careful examination of the cellular changes of the uterus suggests that there are many reasons why adenomyosis could cause infertility. These new studies will also be very important in helping scientists figure out what type of treatments might cure adenomyosis, or better yet, prevent it from developing at all.
What Is the Treatment for Adenomyosis?
The medications Lupron or Synarel can cause cessation of the periods and associated menstrual cramping and even lead to shrinkage of the swelling associated with adenomyosis. However, the effect is temporary-when the medication is discontinued, the symptoms return. At the present time, the only treatment for adenomyosis is surgery. In situations where the adenomyosis is confined to isolated areas in the muscle wall, an attempt may be made to surgically remove these areas and repair the rest of the uterus. In situations where the majority of the uterus is affected, hysterectomy may be the only cure.
Can Uterine Artery Embolization Be Used to Treat Adenomyosis?
Only a small number of women with adenomyosis have been treated with uterine artery embolization (UAE), and the results so far have been disappointing. Symptoms appear to improve for a year or two, but most women then have recurrence of symptoms. Adenomyosis is defined as the presence of uterine lining cells within an otherwise normal uterine muscle wall. The blood supply to that muscle is normal, unlike fibroids, and should be resistant to the effects of embolization. Again, further research will be needed to see if better results can be obtained.
Treating Adenomyosis with the Progesterone IUD
Adenomyosis has been a frustrating disease to treat; medical treatment with oral progesterone or birth control pills often does not work and uterine artery embolization often fails. Hysterectomy is the only treatment known to be highly (100%) effective. According to a recent study, the progesterone-containing IUD (Mirena) can help with menstrual cramping in about 70% of women. The IUD probably works because it slowly gives off progesterone directly to the lining cells in the uterus and in the uterine muscle wall. Progesterone causes the cells to shrink and produce less prostaglandin, the protein that causes cramping. The most common side effects from the IUD were weight gain (29%), benign ovarian cysts (22%) and lower abdominal pain (12%).If you have pain from adenomyosis, this IUD is probably worth considering.
William H. Parker, MD
Clinical Professor, Reproductive Medicine, UC San Diego School of Medicine
Page last updated: January, 2018