Most women with uterine fibroids have no symptoms or just mild symptoms and do not need treatment. In one study, almost 80% of women who chose “watchful waiting” for their fibroids had no major changes in their bleeding, pain, bothersome symptoms, mental health, general health or activity after one year. After menopause, bleeding stops, fibroids decrease in size and the rate of surgery for fibroids decreases dramatically. So, for some women with fibroids “watchful waiting” will allow treatment to be avoided, perhaps indefinitely.
Treatment will be necessary for women with heavy bleeding that causes severe anemia or, very rarely, for blockage of the ureters (tubes that pass urine from the kidneys to the bladder) by very large fibroids. Some women may also chose treatment for heavy bleeding, pelvic pain or pressure, urinary frequency or incontinence that interferes with their quality of life. But, this decision is for each woman to make based on her own sense of her quality of life. Of interest, one study found that women who chose to have a hysterectomy because of fibroid-related symptoms had worse scores on quality-of-life questionnaires than women diagnosed with high blood pressure, heart disease, emphysema or arthritis.
However, if women are offered a hysterectomy as a first and sometimes only treatment option, they may choose to adapt to their symptoms and stop seeking treatment. If this has happened to you, get a second opinion from a gynecologist who regularly takes care of women with fibroids. Otherwise your symptoms (such as bleeding or pain) may slowly get worse (“symptom creep”) and can lead to fatigue from anemia, increasing discomfort and mental fatigue from concern about your situation.
At present, medications, a progesterone-releasing IUD, endometrial ablation, hysteroscopic myomectomy, laparoscopic myomectomy, abdominal myomectomy, uterine artery embolization and focused ultrasound are all available in addition to hysterectomy for treatment.
Can Fibroids Cause Bleeding Problems?
Women with fibroids may have an increased amount of menstrual bleeding, although many women with fibroids do not have this problem. There are a number of theories as to why heavy bleeding might happen. At the time of the menstrual period, when the uterine lining is shed, the inside of the uterus is raw and bleeding. The uterus has two basic ways to stop itself from bleeding. The first is the normal blood-clotting mechanism that works throughout the body by forming plugs in the blood vessels. However, because the uterus is a muscle, it also has the unique ability to contract and squeeze the bleeding vessels of the uterus, much like stepping on a hose. These contractions are what you may feel as menstrual cramps. One theory suggests that the fibroids don’t allow the uterus to squeeze down properly, so the blood vessels in the uterus stay open longer, and you lose more blood. Also, fibroids produce proteins that make blood vessels grow nearby and other proteins that make the blood vessels expand, so that more blood is lost after menstrual bleeding starts.
Other medical conditions may also cause heavy bleeding or bleeding in between periods. Hormonal changes, polyps, overgrowth of the uterine lining, or, rarely, even precancer or cancer of the uterus can all result in abnormal bleeding. Von Willebrandt’s Disease, a not uncommon subtle abnormality of the blood clotting mechanism can also cause heavy bleeding. Therefore, any abnormal bleeding should be reported to your physician, and you should get a thorough evaluation.
When heavy menstrual bleeding persists over time, your body may not be able to make new blood cells fast enough to replace those that have been lost. Some women with fibroids find that the bleeding is so severe that even iron pills (taken with 1,000 mg of vitamin C to help the iron get absorbed into the bloodstream) cannot correct the problem, and anemia develops. Anemia can result in weakness, fatigue, fuzzy thinking and, if severe, light-headedness. If you have any of these symptoms, treatment beyond iron pills should be considered. Please visit: http://www.gynsecondopinion.com/period.htm for more information.
Can Fibroids Cause Pain or Pressure?
A normal size uterus lies below the pubic bone, well down in the pelvis. It is just under the bladder, just above the rectum, and surrounded by the intestines. Since it is so near to these other organs, growth of the uterus from fibroids may cause pressure or, rarely, pain in the pelvis. The uterus is normally about the size of a small pear and weighs less than one-quarter of a pound. But with fibroids, the uterus will enlarge and can cause an awareness of fullness or pressure. If the fibroids grow toward your back, pressure on the rectum can cause constipation. You may also feel pressure or pain in the lower back or discomfort with activity or intercourse. If the fibroids grow towards the front of the uterus, they can press on the bladder and cause frequent urination. However, fibroids do not cause any permanent damage to any of the organs.
If the uterus gets to be as large as a cantaloupe, it may be seen as a noticeable swelling in the lower abdomen, perhaps even making a woman appear pregnant. While not dangerous, the enlarged uterus may cause enough discomfort or enough visible change for you to want to seek treatment.
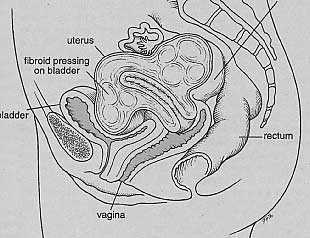
fibroid pressure
Can Fibroids Cause Sudden Pain?
Fibroids are living tissue, and need blood and oxygen to survive. If a fibroid grows quickly, blood vessels feeding the fibroid may not be able to grow fast enough to supply the new tissue with enough blood and oxygen. If this happens, the fibroid undergoes a process called degeneration, or cell death. As the cells in the fibroid die, chemical substances are released that cause pain and swelling in the uterus. This pain may be severe but is not usually associated with any serious problems. If these chemical substances from a degenerating fibroid reach the bloodstream, they may cause a low fever. As some of the fibroid dies, the blood supply to the rest of the fibroid will be enough to keep it alive and healthy. At this point, the pain will go away. This process may take a few weeks. When pain develops in a woman with fibroids, examination by a physician is important to help figure out the source of the problem.
If you have a degenerating fibroid, a heating pad on your abdomen will be comforting, and pain medication should provide relief for a few days or weeks until the pain begins to subside. In rare instances, a fibroid on a stalk (pedunculated fibroid) can twist around on the stalk so that no blood can get through the stalk to the fibroid. If that happens, the entire fibroid begins to die, and the pain becomes very severe and surgery is usually necessary to remove the dying fibroid.
Can Fibroids Cause Urinary Problems?
The uterus lies directly beneath the bladder, and the uterus and bladder are partially attached at one point. If a fibroid begins to grow forward, it may squeeze the bladder so that it cannot fill properly with urine and you may feel the need to urinate more often. Also, when you laugh, cough, or sneeze, the fibroid may push against the bladder and cause you to lose urine. This is called stress incontinence. While this may only be a minor inconvenience for some women with fibroids, others may be so bothered by the incontinence that they limit their activity to avoid embarrassment. There are also other causes of incontinence, so you should get a careful examination. There are now a number of treatments available other than surgery for many of the causes of incontinence. Stress incontinence is not something you “just have to live with”.
William H. Parker, MD
Clinical Professor, Reproductive Medicine, UC San Diego School of Medicine
Page last updated: January, 2018